Benefits Monthly Minute
The August Monthly Minute presents Part II of our mental health parity update and provides highlights of the latest report to Congress on NQTL comparative analyses. While service providers lead the way through mental health parity compliance given their role in group health plan design and operation, the pressure is ultimately on plan sponsors to monitor compliance and navigate enforcement and corrective action.
Part II: MHP Report to Congress: Do Not Pass Go, Do Not Collect $200!
When MHPAEA was amended by the Consolidated Appropriations Act, 2021 (CAA), a provision was added mandating plans to perform and document comparative analyses of the design and application of their non-quantitative treatment limitations (NQTLs) and also requiring the Secretaries of the Departments of the Treasury, Health and Human Services, and Labor (the Departments) to report to Congress annually on the results of their NQTL comparative analyses reviews. Since the CAA’s enactment, EBSA has requested comparative analyses for hundreds of NQTLs and obtained corrections for violations. And, according to this year’s MHPAEA Comparative Analysis Report to Congress released late last month, the Departments have increased their focus on NQTL enforcement efforts.
As previously reported in the February 2022 Monthly Minute, the January 2022 Report to Congress noted four general priority areas of NQTL enforcement. Two additional areas were added to the July 2023 Report to Congress as follows:
- Prior authorization requirements for in-network and out-of-network inpatient services;
- Concurrent care review for in-network and out-of-network inpatient and outpatient services;
- Standards for provider admission to participate in a network, including reimbursement rates;
- Out-of-network reimbursement rates (methods for determining usual, customary, and reasonable charges);
- Impermissible exclusions of key treatments for mental health conditions and substance use disorders (NEW); and
- Adequacy standards for MH/SUD provider networks (NEW).
As noted above, EBSA is placing increased priority on NQTLs related to network adequacy, particularly provider network composition and participation standards, which includes reviewing how plans set provider reimbursement rates and efforts to monitor the adequacy of provider networks. Additionally, EBSA encountered more total exclusions of key treatments for mental health/substance use disorder (MH/SUD) conditions than expected, such as ABA therapy to treat ASD, medication-assisted treatment (MAT) and medications for opioid use disorder (MOUD), and nutritional counseling for eating disorders.
The following table summarizes the specific types of NQTLs for which EBSA requested analyses during this past reporting period:
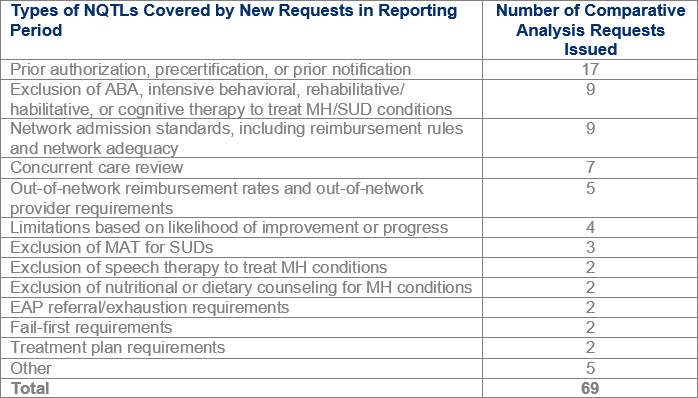
Not only did the new report offer details as to the types of NQTLs that were examined, but it also shed light on the types of corrections that were implemented in response to problematic NQTLs which included –
- Removal of exclusion for MH/SUD residential treatment facilities and claims reprocessing.
- Ending the use of an EAP as a gatekeeper for MH/SUD services.
- Removal of exclusion of coverage for MH/SUD telehealth benefits.
- Removal of prior authorization requirement on certain MH/SUD services. Notably, EBSA views removing impermissible limits on access to SUD treatments as an urgent enforcement priority in light of the opioid epidemic.
- Removal of exclusion for treatment provided by opioid treatment programs and reprocessing of claims.
- Removal of exclusion of drug testing for MH/SUD conditions and reprocessing of claims.
- Removal of exclusion for inpatient substance use disorder treatment unless the participant completes the entire course of treatment.
- Removal of ABA therapy exclusion.
Apparently, in its second year of CAA implementation, EBSA did not see a marked improvement in the sufficiency of the initial comparative analyses received – indeed, none were found to be sufficient by the EBSA. The same deficiencies and trends noted in the January 2022 Report were still commonly reflected. Where analyses were made available for review, they frequently failed to –
- Adequately explain how factors were applied when determining which benefits would be subject to the NQTL. Deficient explanations of the application of a factor were compounded by inadequate definitions of factors and inadequate explanations of how sources were used in selecting, defining, or applying factors.
- Demonstrate how or if the factors were comparably applied to MH/SUD benefits and to medical/surgical benefits.
- Adequately explain how an NQTL was applied in operation, and instead described processes generally and evaluated differences in application to MH/SUD and medical/surgical benefits without sufficient detail.
- Demonstrate that, in operation, the NQTL was comparably applied to both MH/SUD and medical/surgical benefits.
Further, notwithstanding the CAA’s requirement for all plans to have prepared an NQTL analysis by February 10, 2021, many plans were unprepared to submit their analyses upon request. And, when plans that were initially unprepared ultimately submitted comparative analyses, they often lacked data showing what happened when the NQTL was applied in operation. When operational data were included, plans often failed to explain numerical inputs, underlying methodologies, or calculations behind summary data that were presented as evidence of a comparable application.
And, despite the fact that more plans identified specific factors used in the design or application of the NQTL, EBSA noted the lack of meaningful analysis of the NQTL’s design and application. For example, even when comparative analyses listed factors considered in the NQTL design, many did not explain how the plan applied each factor. Also, where analyses listed more than one factor, there was no explanation about how the factors worked together. And, while some comparative analyses identified factors and defined each factor with some explanation about its application, many failed to demonstrate that the factors were applied in a comparable manner. Notably, EBSA claimed to have received incomplete responses when asking for supporting documentation, and as a result, questioned whether comparative analyses were accurate reflections of plans’ processes.
The new report also stated that many comparative analyses did not include a sufficiently detailed explanation of how the NQTL was applied in operation to the specified benefits and noted that the relevant information necessary to demonstrate comparable application depends on the type of NQTL, how it is applied, and other unique details. EBSA observed three common ways that plans fell short when attempting to demonstrate comparable application of an NQTL in operation:
- Lack of data showing results when the NQTL was applied in operation;
- Failure to explain numerical inputs, underlying methodologies, or calculations behind summary data presented as evidence of comparable application; and
- Failure to explain apparent differences in access to MH/SUD benefits as compared to medical/surgical benefits.
In general, EBSA responded to deficient comparative analyses by giving plans opportunities to supplement responses and cure deficiencies. Although EBSA bemoaned the process as time-consuming and resource-intensive, in some instances, it resulted in plans satisfying EBSA’s NQTL inquiry altogether. Apparently, data showing the effect of an NQTL’s application were particularly important and sometimes operated as a “green flag” signaling that an NQTL in question did not appear to apply more stringently to MH/SUD benefits relative to medical/surgical benefits. (Specific examples of how some plans cured deficiencies identified in insufficiency letters by providing detailed additional information were included in an appendix to the report.)
KMK Comment: The Departments’ persistent review of NQTL analyses is breaking new ground in the area of mental health parity and enforcement. EBSA is prioritizing potential violations that stem from the actions of service providers that affect not just one plan, but hundreds or thousands of plans. These new enforcement efforts are resulting in the removal of exclusions, revised comparative analyses and broad corrective actions. Considering the fact that EBSA develops investigative leads through plan reviews and from multiple sources (state and federal regulators, media, private litigation, participant or beneficiary complaints, professional associations, and patient advocacy groups), it is essential that plan sponsors work closely with counsel and service providers to diligently review plan documents and administration for mental health parity compliance, keep up-to-date on their NQTL comparative analyses, and carefully respond to requests for plan information, governmental audits or exams, and related inquiries.
The KMK Law Employee Benefits & Executive Compensation Group is available to assist with these and other issues.
Lisa Wintersheimer Michel
513.579.6462
lmichel@kmklaw.com
John F. Meisenhelder
513.579.6914
jmeisenhelder@kmklaw.com
Antoinette L. Schindel
513.579.6473
aschindel@kmklaw.com
Kelly E. MacDonald
513.579.6409
kmacdonald@kmklaw.com
Rachel M. Pappenfus
513.579.6492
rpappenfus@kmklaw.com
KMK Employee Benefits and Executive Compensation email updates are intended to bring attention to benefits and executive compensation issues and developments in the law and are not intended as legal advice for any particular client or any particular situation. Please consult with counsel of your choice regarding any specific questions you may have.